A Heart Attack in 1965 Could Kill You. The Same One Today Probably Won't.
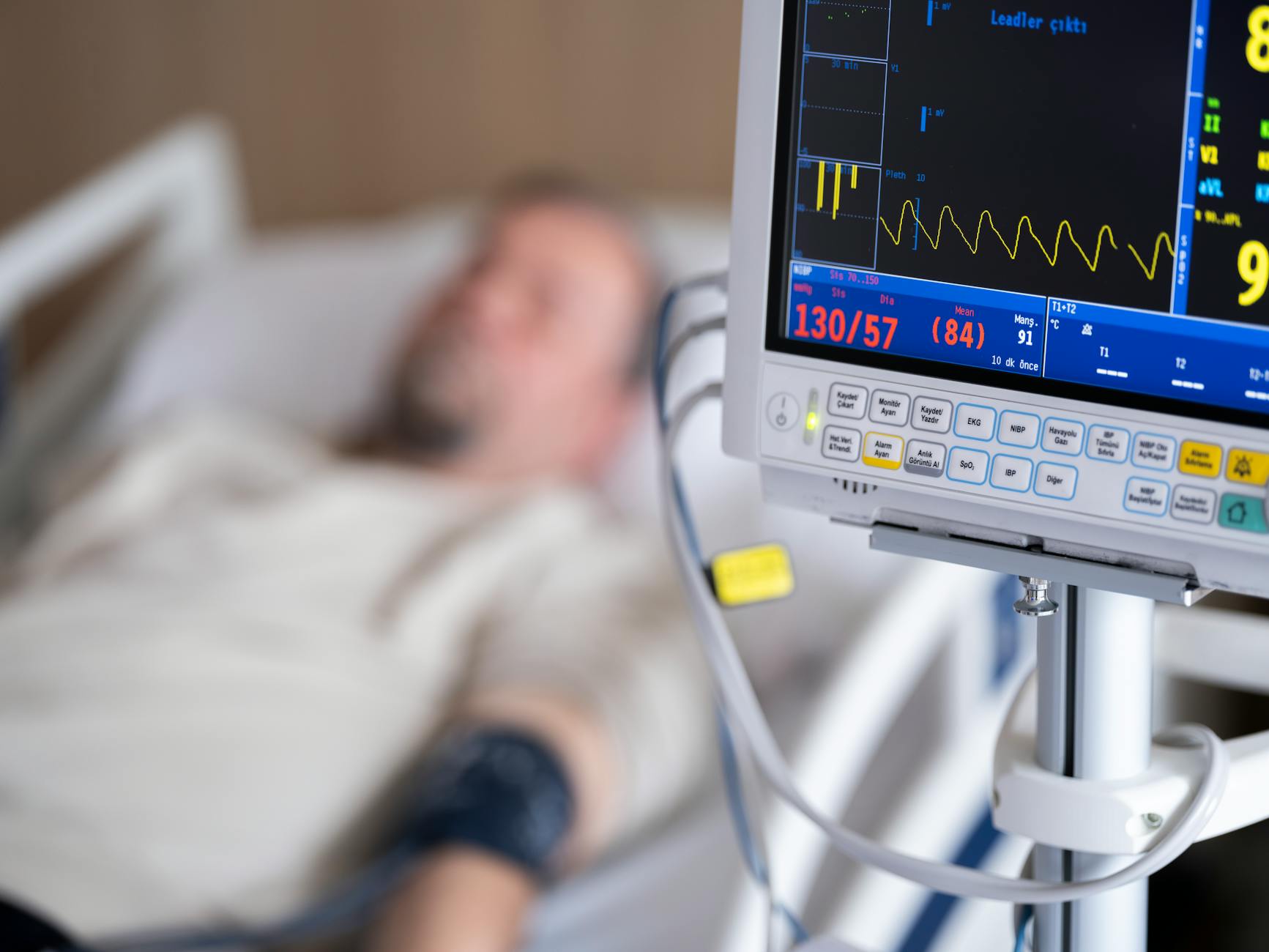
A Heart Attack in 1965 Could Kill You. The Same One Today Probably Won't.
Picture your grandfather — or maybe your great-uncle, or a neighbor from the old neighborhood. A man in his late fifties, working a physical job, eating the way everyone ate back then: red meat, butter, cigarettes with his morning coffee. One afternoon, he grabs his chest. His face goes gray. Someone calls the family doctor.
What happens next would be almost unrecognizable to a cardiologist practicing today.
What a Heart Attack Looked Like in the 1960s
In 1965, if you survived long enough to reach a hospital, the treatment was essentially: lie still and hope. Physicians prescribed bed rest — sometimes for weeks — along with aspirin, oxygen, and mild sedatives to keep the patient calm. The underlying blockage, the actual clot strangling the heart muscle, was left completely untouched. Doctors simply didn't have the tools to reach it.
Hospital mortality rates for heart attacks hovered somewhere between 25 and 30 percent. That means roughly one in four people who made it to the emergency room still didn't make it home. And for those who did survive, the damage was often permanent. Large sections of heart muscle died during the event, leaving patients weakened, short of breath, and told to avoid exertion for the rest of their lives.
There were no cardiac care units until the mid-1960s, and even then, they were rare. Defibrillators existed in research settings but weren't widely available. The EKG was used, but what physicians did with that information was limited. Essentially, medicine could watch a heart attack happen. It just couldn't stop one.
Many men — and it was disproportionately men being treated, since heart disease in women was dramatically underdiagnosed — never returned to work. A heart attack at 60 often meant the end of an active life, full stop.
The Revolution That Changed Everything
The shift didn't happen overnight. It came in waves, each decade bringing something that would have seemed like science fiction to the generation before.
The 1970s brought coronary bypass surgery, allowing surgeons to literally reroute blood around a blocked artery. The 1980s introduced clot-dissolving drugs called thrombolytics — medications that could chemically break up the blockage that was killing the heart muscle, if given quickly enough. Then came the real game-changer: balloon angioplasty and, eventually, the coronary stent.
A stent is a tiny mesh tube. During a procedure called a percutaneous coronary intervention (PCI), a cardiologist threads a thin catheter through an artery in your wrist or groin, navigates it all the way to the blocked vessel in your heart, and deploys the stent to prop the artery open. The whole thing takes roughly an hour. Patients are often awake during the procedure. Many go home the next day.
The blockage your grandfather couldn't survive? It's now treated before breakfast.
The Same Crisis, Sixty Years Apart
Let's run that side-by-side comparison directly.
In 1965, a 58-year-old man clutches his chest at home. By the time an ambulance arrives — if one is called at all — significant heart muscle may already be dying. At the hospital, he's given aspirin, told to rest, and monitored. If he survives the first 48 hours, he spends three weeks in a hospital bed. He goes home fragile. His doctor tells him to take it easy. He probably never shovels snow again.
In 2025, a 58-year-old man feels chest pressure during dinner. His wife calls 911. Paramedics run an EKG in the driveway and transmit results to the hospital before they even leave the block. The ER team is assembled and ready when he rolls through the door. Within 90 minutes of symptom onset — the current benchmark for what's called door-to-balloon time — a cardiologist has opened the blocked artery with a stent. He's in a cardiac care unit overnight, walking the hallway by morning, and home within 72 hours. His heart muscle, caught in time, is largely intact.
The survival rate for heart attacks in the US today exceeds 90 percent. That number would have been incomprehensible in 1965.
Why This Feels Personal
Here's the thing that makes this more than a medical history lesson: almost all of this progress happened within a single human lifetime.
If your father or grandfather had a heart attack in the 1960s or 70s, he faced a fundamentally different odds sheet than you would today. The men who didn't make it — and there were millions of them — weren't unlucky in some abstract sense. They were simply born too early for the tools that now exist.
And those tools keep improving. Newer stents resist re-blockage. AI-assisted imaging can identify vulnerable plaques before they rupture. Medications like statins, beta-blockers, and PCSK9 inhibitors have reshaped what it means to manage heart disease long-term.
The heart attack hasn't changed. The body's vulnerability hasn't changed. What changed is everything around it — the knowledge, the technology, the speed of response.
Your grandfather faced the same crisis you might face someday. He just faced it in a different world. And that difference, measured in survival rates and second chances, is one of the most quietly staggering transformations in the history of American medicine.